Cigna Weight Loss Surgery Requirements & Free Insurance Check. READ THIS FIRSTEven if your insurance company covers bariatric surgery in some plans, that does not mean that your specific plan covers it.
The obesity surgery approval requirements in this section assume that weight loss surgery is covered by your specific policy. To confirm whether your specific policiy covers bariatric surgery, click here to contact a surgeon and ask for a free insurance check. Disclaimer: The information contained on this page may not include all components of your insurance company’s medical policy and/or may not be up to date. Contact your insurance company to confirm all benefits. In order to be approved by Cigna Health Insurance for bariatric surgery in the United States, you must meet the following criteria: The individual is at least 1. OR has reached full expected skeletal growth AND has evidence of EITHER of the following: Diagnosis of Morbid obesity, defined as: A Body Mass Index (BMI) greater than 4.

Considering weight loss surgery? As you do your homework to see if it's a good choice for you, you'll want to learn about the various types of operations. Does Medicaid pay for bariatric surgery? Medicaid programs cover bariatric surgeries for some patients under circumstances that are very close. CMS no longer requires that covered bariatric surgery procedures be performed in facilities. Northwest Weight Loss Surgery: 50. Medicaid Services. BCBS Alabama does cover weight loss surgery as long as your policy does not exclude coverage. ObesityCoverage strongly feels that morbid obesity is a disease and. Information about insurance coverage for gastric bypass surgery. Explanation about obesity and how it relates to various insurance limitations.
A BMI (Body Mass Index) 3. Mechanical arthropathy in a weight – bearing joint. Type 2 diabetes mellitus.
Poorly controlled hypertension (systolic blood pressure at least 1. Hg or diastolic blood pressure 9.

Hg or greater, despite optimal medical management)Hyperlipidemia. Coronary artery disease. Lower extremity lymphatic or venous obstruction. Obstructive sleep apnea. Pulmonary hypertension.
Below are some questions people often ask about Medicaid benefits. Alabama Medicaid does not. Alabama Medicaid covers this type of bariatric surgery for. Does Anyone Know if Alabama Medicaid covers Lap-Band. Does Alabama Medicaid cover the cost of. It appears that bariatric surgery is covered under Alabama. Does Medicaid Cover Gastric Bypass Surgery in. I'm Sharon, Medicare Coordinator for BeLiteWeight. I am a weight loss surgery patient myself and it has given me the ability to lead a much more active lifestyle.
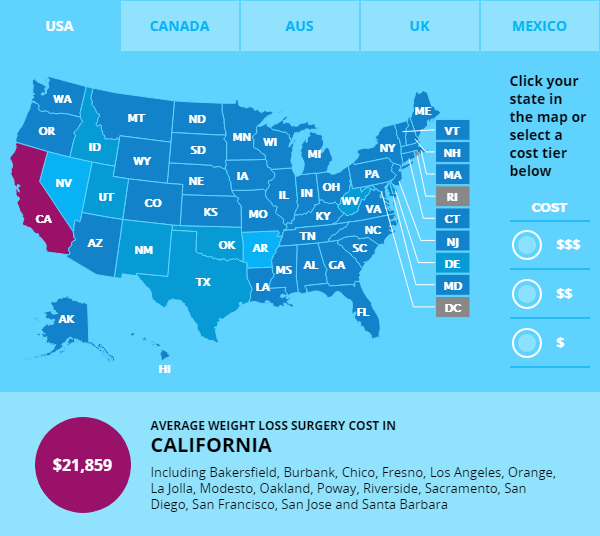
Reviewed by Neil Hutcher, MD. Weight loss surgery is both complex and costly. For example, the average cost for the gastric bypass procedure ranges from $18,000 to.
Use this BMI Calculator to check your body mass index: Medical management including evidence of active participation within the last 1. The weight – management program must include monthly documentation of ALL of the following components: Weight. Current dietary program. Physical activity (e. Medical Management & Other Weight Loss Programs. Programs such as Weight Watchers. However, physician- supervised programs consisting exclusively of pharmacological management are not sufficient to meet this requirement.
A thorough multidisciplinary evaluation within the previous six months which includes ALL of the following: an evaluation by a bariatric surgeon recommending surgical treatment, including a description of the proposed procedure(s) and all of the associated Current Procedural Terminology (CPT) codes. A separate medical evaluation from a physician other than the requesting surgeon that includes a recommendation for bariatric surgery. Unequivocal clearance for bariatric surgery by a mental health provider. A nutritional evaluation by a physician or registered dietician. Revision Requirements.
Reoperation and Repeat Bariatric Surgery – Cigna covers surgical reversal (i. Cigna covers revision of a previous bariatric surgical procedure or conversion to another medically necessary procedure due to inadequate weight loss as medically necessary when ALL of the following are met: Coverage for bariatric surgery is available under the individual’s current health benefit plan. There is evidence of full compliance with the previously prescribed postoperative dietary and exercise program. Due to a technical failure of the original bariatric surgical procedure (e. UGI) series or esophagogastroduodenoscopy (EGD), the individual has failed to achieve adequate weight loss, which is defined as failure to lose at least 5. The requested procedure is a regularly covered bariatric surgery.


If Your Policy Does NOT Cover It: Seek Partial Coverage. You may be able to get part of the costs paid for by insurance even if weight loss surgery isn’t covered. It’s all about how your doctor and hospital submit your claims to your insurance company.
For example, there are many non- bariatric surgery reasons for your doctor to recommend: Cardiology exam. Lab work. Medically supervised diet program. Psychological exam. Sleep study. These are ordered for many reasons other than bariatric surgery and may be covered as a result. If your doctor submits one of these claims using a weight loss surgery CPT code (Current Procedural Terminology Code), your insurance is unlikely to cover it. After all, these tests will be beneficial regardless of whether you move forward with surgery.
 RSS Feed
RSS Feed
